having a bunionectomy and osteotomy procedure - A personal bunion Surgery story (hallux valgus)10/25/2022 Just mentioning the word bunion makes me wince for various reasons - not just because of the stigma attached to them, how unsightly they are, or the unbearable pain, but also because they are so much more than a bump at the side of the foot. It's a common condition; many people have bunions and you will find that nearly everyone recognises them. There is an element of shame or embarrassment, in my opinion, that comes along with them. People think you have acquired bunions because of your penchant for wearing high heels. The 'older' population often have them - so they can make you feel a little less youthful in some ways. They can be very unsightly - making the best of us want to hide our feet away. Finding the right shoe to wear can become an impossible task, as virtually every single pair causes more pain. Even laying in bed can be uncomfortable as just a small amount of pressure on the side of the foot can create discomfort. Walking, regardless of foot attire, becomes a pain endurance event and leaves you with even redder, more aggravated feet that stay inflamed and angry for days. I am not a medical professional. I am a Sports Massage Therapist. I have had bunions since my twenties. If you would like to know my bunion story read on... I found it helpful to read other people's bunion stories when I was deciding how to treat my own. In fact, to be honest, I was a bit shocked that there was not so much out there. Maybe, this account will be useful for some people. Please only use my personal bunion account as food for thought, to help you think about your own condition and to help start your own thought processes about what you might like to do about your own feet. Always seek advice from a medical professional. Do not suffer in silence - find out what options are available to you, think about how badly this condition affects your life and what you would like to try to obtain relief. Bunions are thought to be acquired by wearing high heels as they tend to put pressure on the MTP joints (the metatarsal phalangeal joints). These are the joints at the base of the toes - the equivalent of your knuckles for the want of a better description. The 1st MTP joint is your big toe joint. This area takes a lot of weight from the body. Hallux Valgus is the medical term for bunions. A bunion is actually a misalignment of the toe, starting from movement of the bone that comes before the toe (the metatarsal). The joint at the base of the toe becomes displaced/dislocated. There is a bursa (a fluid filled protection sac) on the side of the foot at the bunion location and this can become inflamed; leading to more swelling, redness, discomfort and an even bigger protrusion at the side of the foot. The part that sticks out is actually the head of the 1st metatarsal - the medial part (inner side) of this joint. Just think if your finger was dislocated, it would be all hands to the deck to sort it out, but when it is your big toe, the most weight bearing toe, we all just sit back and say, 'Oh, I have a bunion...' Yet this has implications for us. The list of possible causes are varied and not known for sure. They are thought to include wearing narrow and tight fitting shoes, wearing high heels, genetics, having a laxity of the MTP joint (naturally and because of stressors to it) and having a tight tibialis anterior muscle. Muscles and tendons have a huge impact with the way the joints move - our biomechanics. Some people may be more predisposed because of the shape of their foot. Some feet have a dropped or lower arch - transverse or longitudinal. One Surgeon, that I listened to whilst briefing his bunionectomy patients prior to considering surgery, said that he believed that high heels were unlikely to be a cause, as men also suffered from this deformity of the foot. That point of view is very interesting for me to hear. There are different degrees of bunion / Hallux Valgus. I have seen them referred to by grade and by mild, moderate and severe categories. Mild deformity shows a small amount of deviation of the toe. Moderate deformity shows a little more of the toe leaning towards the next toe and more of a bump is visible on the inside of the foot. A severe deformity is the final stage, where the bump is very exaggerated and the toe deviation is more acute - there might even be toe overlapping. In some cases, the MTP joint at the base of the toe can become arthritic, as a result of the long term misalignment of the joint and damage to it's cartilage. The big toe can also cross the second toe. The condition can progress through the stages. It is worth keeping an eye on your feet to see if there is deterioration. Taking a photograph may help with this. Treatment options vary from the more conservative options to surgical procedures and can include:
Wider fitting, flatter shoes made of a softer material became my preferred options, but did not give me enough comfort as my condition progressed. I would still end up with sore feet and the pain would last for several days - even causing me a problem when I was in bed. Sometimes I had to use a pillow or bolster, to stop the side of my foot making contact with the mattress. Even fabric shoes caused discomfort and became an issue for me when I was working. My running shoes were always a brand that had a wider toe box and yet I had to look out for additional things such as raised/solid edges on the side of the shoe, bonded logos or aesthetic attachments and seams on the inside of the shoe. I was in Runner's Need in Covent Garden for three hours choosing a comfortable pair of trail running shoes and I still ended up with a pair that rubbed my bunion raw. The first time I took a short run in the new shoes, I had to run home barefoot and wear Compede second skin patches for the next few weeks. I had to tape up the inside seam and wear a silicone bunion protector to be able to use that running shoe again. I had the same issues with my inline skates. I used to have lessons for inline skating general skills and tricks - such as skating around cones. I needed a solid boot to give my ankle and foot the full support for the skating tricks. The solid boot caused my bunions a lot of discomfort and I had to wear silicone pads to protect my foot - the pads had to be taped down to stay in place. The pain was still unbearable and I had to upsize by two whole sizes of skate to be able to wear a solid skate boot. I had an overspill of foot when wearing some sandals and flip-flops. Sometimes I would hit the side of my foot against pebbles. Actually, even barefoot, I would hit the sides of my feet together or against things as the bone just stuck out so much. I knew the condition deteriorated further when other parts of my feet became affected - the other toes started to misalign and my left foot had pain at the MTP joints of the smaller toes. I was never one for wearing very high heels - maybe just for the odd special occasion and for a limited amount of time. I went to work in flatter shoes and the rest of the time I was barefoot or in some kind of sports shoe - horse-riding boots, hiking boots or running shoes. The thing about high heels is that they put our foot in a compromised position and the weight-bearing function is impaired. The arches of the foot cannot do their job properly and the weight of the body moves away from the ideal tripod-based three-point contact with the ground. Much of the body's weight is redirected through the ball of the foot. This pressure is thought to weaken the MTP joint through improper foot mechanics. I should think that the loading on the stretched MTP joint could lead to the joint ligaments becoming stretched and lengthened and possibly contributing to dislocation of the stressed joint. The lower the heel on the shoe, the less acute the loading is on the ball of the foot. Shoes with a wedged sole may give you some height via the heel, but keep the pressure off the forefoot a little better. Silicone bunion protectors act as a little cushion to protect the edge of the bunion. They do not have any remedial action. They can help to stop the bursae sacs from becoming further inflamed and developing bursitis. The bursae sacs act as a cushion for the bone and are easily aggravated by pressure and friction. There are specific bunion protector pads and some even have a spacer between the first and second toe. I improvised with a silicone gel foot pad with an integral toe loop, as it was easier to wear. I also tried bunion splints. There is no evidence to prove that they actually work, but they did provide some temporary relief for me - especially when I had a flare-up. Splints vary in design. My splints had a padded metal bar with two velcro straps that secured around the big toe and the girth of the foot in turn. It was possible to tighten the straps to increase the tension on the big toe. Too much tension created discomfort. Moderate tension gave me some brief, but welcome, respite from Hallux Valgus related pain. These are best worn in bed for a little time or when resting as it is not possible to walk with the splints on. Shoe inserts are a bit of a controversial measure according to some physical therapists. From the prescribed tailor-made ones, to the off-the-shelf kind, expensive and cheaper options are available. I had a Podiatrist make me full-sole inserts following a full assessment and then 3/4 inserts. Both were difficult to wear. There was never enough room in my shoes for them and my feet to coexist comfortably. My toes became squashed against the top of the shoe and calluses formed on them. I had MTP joint supports to help me gain back some transverse arch support and main arch support. Some physical therapists believe that supporting an arch in the centre of the arch does not make sense. Likened to an arched bridge being supported in the centre - looking at the laws of physics, it would make more sense for an arch to be supported at the sides of the arch to be more structurally sound. They recommended learning to use the foot correctly and wearing shoes that allow the natural spread of the toes. My inserts were also quite uncomfortable, despite wearing them for a short amount of time and gradually increasing that time. They were also made from a slightly softer material and the arch height was calculated specifically for my feet. It is always best to consult with a professional and have orthotic insoles made specifically for your own feet and in conjunction with the shoes you plan to wear them with. Exercises for the feet can also be followed - the podiatrist will advise you according to your specific needs. General foot strengthening exercises like picking up socks with your toes, and lifting your big toe, and then the remaining four toes as a unit, whilst keeping your foot flat are always helpful. Stretching out the soleus, the gastrocnemius and the tibialis anterior muscles is always a good idea too. The more medical-based interventions include taking some kind of anti-inflammatory medication and surgery (seek advice from your health-care provider). Having a bunion operated on is not to be taken lightly - there are a variety of methods depending on the severity of your condition. I had quite a big procedure in terms of an osteotomy, ligament release and a reinforcement rod. I will talk about this more... I have my own beliefs about how my bunions were caused. When I was in my early twenties I held a black belt in Ki Aikido. We had a guest instructor visit from abroad and work with us for a weeklong period. He performed a test on me to see if he could unsettle my concentration and he could not do so. He consequently struck me very hard and abruptly on the chest. I was in a kneeling position up on my toes. I fell backwards overextending all of my toes with my full bodyweight, and with great momentum and force. All of my MTP joints partially dislocated. I had never seen a technique executed in this way and I believe it was unnecessary, unethical and driven by ego. How my daily life was affected... I had great pain whist walking and absolutely no shoe could prevent this exacerbation of symptoms. The increase in pain that followed would last for days. I could never find suitable running shoes - I would hunt around for a shoe with a wide toe box constructed of softer material. Shoes that appeared to be fine in the shop, would then cause me a problem during my run. Feet expand during running and trying something on in a shop cannot be compared to running with the same shoe on. I usually ended up upsizing to try and gain some extra width. Special occasions were a nightmare because of pain, standing for a long time and walking and dancing. Whichever shoe I wore caused some kind of an exacerbation of symptoms and the side of my foot would be bright red and painful for days. I even had pain during work and I would shift my balance trying to gain relief whilst I was massaging. I wore plain fabric leisure shoes, but even with the soft, lighter fabric, I was still feeling uncomfortable. Some of my clients noticed and remarked that my shoes were not suitable - they could see my bunion pushing through the shoe. I actually could not find any shoes that were suitable. I used to love massaging barefoot, but I had to stop when my toe deviation became so extreme, that I was scared to show people. My balance was affected as my gait/foot biometrics had become altered. I was no longer able to balance adequately using the big toe for the main stability of the foot. Even my walking gait had become affected. In my sports and whilst walking, I tended to lose my balance at times. I was very embarrassed by the sight of my feet. I had to buy shoes that would cover the bumps on my feet. I hated certain people seeing me barefoot. I was trying to hide my feet in photographs. I hated the stories everyone told me about the other people they also knew with bunions and how severely affected they were with their overlapping toes. That's not to even mention the stories about their parents with bunions and their operation stories. Frequently, I found myself apologising about how my feet looked. My friend who is a Surgeon was coming to run with us. He came to the house to catch a ride. I was barefoot - I mean, who wears their trail shoes in the house? I found myself talking about my feet when he saw them and feeling so self-conscious. There was a lot of pain in my kickboxing classes - especially during push kicks; sometimes I would be wincing out aloud and unable to continue until the pain subsided. I also found lunges difficult - any movement involving the ball of the foot created vast amounts of discomfort. My sleep was so disturbed - I often had to use a pillow to stop the sides of my feet touching the mattress. I would wake up because of the pain. When I was walking, the sides of my feet would knock against each other - regardless of whether or not I had shoes on. I would hit pebbles on the beach with the bump at the side of my foot, which was extremely painful. These are the things that I tried:
How my case was dealt with: I saw my Doctor and he made a referral for me to see an Orthopaedic Specialist. The Orthopaedic Doctor had a quick look and said that they perform operations to correct the toe and that I was eligible. He said that they would preserve the articulation in my foot and put a metal rod into my foot for a month. That I could walk with a special shoe and that one month off work would be necessary. I needed both feet to be operated on, but he said we would start with one, so that I could still get around. He sent me for an x-ray. I asked the receptionist what the next step was and he said the Doctor would be in touch about the operation date. I waited a few weeks and did not hear back from them. Meanwhile, my Specialist had sent me for an MRI for my knee and whilst I was having the follow-up appointment for the results, I was given the operation date for my foot by another Receptionist (after I also asked them for advice about how I would be notified of the operation date). Two days prior to surgery I went back to have some pre-operation checks and screenings - I had a PCR test, general blood tests, a chest X-Ray, a heart ECG and a meeting with an Anaesthetist - we talked about allergies, medications, my general health, checked my teeth, listened to my lungs and we discussed anaesthesia, sedation and pain relief. She recommended a spine block rather than a General Anaesthetic, but she said I should discuss it with the Anaesthetist on the day. The tests and checks were very thorough. I was told to eat bland foods that would not make many gases, such as white macaroni and halloumi cheese (I am Cyprus based folks!), for my last meal before 6pm the evening prior to surgery. I was allowed to continue to drink water until the morning, but I stopped about 4am to be sure I was safe. The time to arrive for surgery would be given to me the day before the operation. On the day of the Surgery, I arrived a little earlier than I was told to arrive. I went into the hospital, checked in with my ID card and filled out a form. They found my PCR results on the computer system. I sat outside the hospital waiting to be called in for quite a while. I was hungry and nervous. The close friend who drove me to the hospital sat with me until I was called in. I was taken to a ward and shown my bed. They gave me a gown and asked me to undress. The put the catheter into my arm. I signed an operation consent/disclaimer form. My allergies were checked and recorded once again. I waited until it was my surgery time. The Nurse put me at ease. I was taken to Theatre in my bed as there were not any wheel chairs available. I had to wait in the corridor until there was space for me to slip into the recovery room for a few minutes and there was no waiting area available for me pre-operation. In the corridor, a Surgeon came to see me. He was very serious and 'in the zone'. He asked which foot we were operating on and whipped back the sheet to check my foot out. When I said the right, he asked why as the left was worse. He flexed all of my toes - all ten toes are maligned. He disappeared. When I was in the recovery room, the Anaesthetist arrived. He was in the zone too - very serious and to the point. He advised me to have the nerve block, checked my allergies once again, and asked about sedation. I told him that I did not want to be too aware of what was going on, but that it was up to him as the specialist to decide on how sedated I should be. I was taken into the Theatre room and transferred onto the operating table. I sat up and bent over a pillow whilst a Theatre Nurse supported me in order for the spinal block to be administered. I was very nervous. I was aware of a puncturing sensation in my spinal area, like a pop, as the needle penetrated a membrane. I thought that was it, but then he said the next step would hurt a bit. I felt pain as the nerve block was administered. Immediately, I sensed an altered sensation in my legs. I laid down. The effect grew in intensity. I was then asked how much I weigh, an oxygen meter placed on my finger tip and electrode pads were applied to my chest. I do not remember anything else as the Anaesthetist then gave me a full sedation. When I woke up I had an oxygen mask on and this was removed. The operation took about an hour. I was then taken into the Recovery Room for a little while and observed. Nurses then took me to an X-Ray room. I was still a bit out of it from the sedation. The Radiographer needed to place my operated foot flat for the X-Ray. I do not know if she was aware of the operation that I had done. The Nurses helped her bend my knee and place my foot flat. Of course it would not stay flat as my entire leg was numb from the spinal block. The leg immediately fell outwards and smashed out of control against the safety rails of the bed. The Radiographer was laughing - she found it very funny. I made a shocked squealing sound and looked very concerned. I was very shocked by what just happened - it seemed very negligent to me and I was worried that damage may have been sustained. I really thought that in my vulnerable state I would be looked after by the two accompanying Nurses. I had not long woken up from heavy full sedation. They all lifted my leg once again, bent my knee and then the radiographer tried to prop my foot up with a gallon tank of water - against the toe that had just been operated on. This is the toe that had an osteotomy - a large piece of bone removed from the metatarsal and was being held together by a metal rod, with a gap between the two pieces of metatarsal bone shaft. Think chicken souvkali on a stick with the meat parted and you will understand how my toe was literally suspended on the rod - quite like a lollipop... I realised that the young Radiographer had little experience in knowing how to safely X-Ray my foot, and to be fair, maybe she was not adequately briefed. I said no to her and did a sit-up crunch, and held onto my own leg to keep it in place. She asked if I could manage and I did. It was not ideal post surgery and my leg was heavy to hold as it was totally numb. I train and have a good level of strength - I do not think every other person would have been able to hold their leg in this way. I would think and hope once the Radiographer saw the X-Ray she would have learnt a lesson from this. I also hope the Nurses would have spoken up about the incident - which would have potentially had a very bad outcome if I had not stopped my operated foot being propped up by a gallon tank of water in the weakest aspect of it... I was taken to my room on the Orthopaedic Ward. The staff were very good on the ward. They made me comfortable, brought me water and gave me a meal. The Surgeon then came to visit me. He asked where my surgical shoe was and I explained that I did not have one. I thought that the hospital would supply me with one. The Surgeon said that they would sort something out in the morning. He said that they removed a piece of bone from my metatarsal and that my big toe alignment had been corrected. He said that the joint was fine and that there was no arthritis present. He also said all of my toes were out of alignment and that I would potentially need the same procedure for all of the toes, but we would see if this procedure was enough in the first instance. He apologised that my Surgeon was absent due to some kind of emergency and that he had had to step in and perform the surgery. I asked the Nurses how I would manage to get to the bathroom and they brought me a zimmer frame. I had to hop with the frame - I was not allowed to put my foot down at all. I was so dehydrated that I did not need to use the bathroom until late afternoon. The Nurses had to walk along with me to make sure I was safe. One had to help me in the bathroom too - which I was a bit mortified by, but what can you do... I managed to get out of the bathroom on my own though. To be honest, if I had not been training so hard, I do not think I would have been strong enough to sit on the toilet and stand back up with only one leg - there were no grab rails in the bathroom. The zimmer frame was a great help in supporting me whilst I hopped along, but it was of more limited safe support as I was sitting and standing. Bare this in mind if you have the same/a similar procedure - that surgical shoe, if you are allowed/told to wear one, will be your lifeline. You will literally have to wear it for every step you take to ensure you keep your weight off the forefoot/mid-foot and make sure you do not end up back in theatre again. The Anaesthetist then came to see me too. He was thorough in checking how I felt and whether I was okay post spinal nerve block and sedation. He also checked if my leg sensation had returned by pushing down on my thigh a few centimetres above the knee. He chatted to me for a while and explained that he opted for a full sedation as he could tell that I was very anxious. I had a funny recollection about something that I thought happened in the operating theatre and I spoke to him about this. I have some odd vague recollection about wanting to see what they were doing and pulling at a curtain drape to see: the Anaesthetist laughed and smiled, he said that I would have been able to hear things, but I would not have been able to understand what was happening. I must have been sedated to a dream state level. I did not have any side-effects from any of the medication administered. I had a headache, but this eased off as I hydrated. I was in pain and the foot felt extremely swollen. There was a lot of protective padding wrap and bandage. It was hard to see how much oedema was actually there. I could not feel my toes, the sensation came back to my toes a few days later - whether this was due to oedema or the spinal nerve block I do not know and to be honest, I did not realise that this had happened until I could feel my toes once again. I spoke to the Nurse about the pain, despite the IV pain treatment. The Nurse explained it was the hardware they had placed in my foot and gently touched the top of my foot (above the arch) - I gasped in pain and she was shocked. Now it makes sense as this was the region of the metatarsal osteotomy - where they had removed a cross-section of the bone. There was a visiting time and the Nurse asked me who was coming to see me. I am single and my close family is in the UK. My extended family is in another City in Cyprus. No-one was coming to see me. I felt my eyes fill with tears. The Lady next to me had her Husband come to see her. When he left, I thought that it was silly for both of us to lay next to each other without speaking and offering each other support, so I spoke to her and asked her how she was feeling. We I could not sleep that night. The pain was excruciating and I tossed and turned trying to find a position that offered me some respite. The room was also freezing. I also kept getting up to use the bathroom - I finally had managed to hydrate! When I did fall asleep, the other patient was up trying to get to the bathroom and she was also in pain and talking about it. When we both settled down, it was 5 am all of a sudden and we were woken up to have our pain medication administered again. That is hospital life I guess. The following day, another Doctor came to see me and told me that I would be discharged in the next hour. We spoke about the surgical shoe again. He said in a very very firm voice, that under no circumstances was I permitted to take a single step without the surgical shoe. He gave me a discharge letter and informed me that I had to come back to the Outpatients Department on the Monday and have the dressing changed. He also said that I needed to take a daily anti-thrombosis shot for 30 days and that the prescription was on the system. I was also signed off from work and eligible to sign up for sick-leave. He said he would find out about the surgical shoe. I frantically Google searched for the surgical shoe. It was about 11am. I knew that shops selling orthotics would be closing within the next two hours. I did not take much cash with me to the hospital and I left my credit card at home. I was starting to panic. I asked the Nurse once again for help. She came back with a leaflet and circled the shoe that I needed to order. I called up the establishment called K.O.E. and they were so helpful. They brought two pairs of surgical shoes for me to try on directly to my hospital bed within 40 minutes. The surgical shoe needs to be fitted properly - the toe needs to be protected by the length of the shoe and your weight in the heel area. The velcro strap around the heel area gives support and the veclro around the foot secures your forefoot - this must not be too tight or too loose. As the day goes on, you might need to let the velcro out a little as the foot swells. The shoe was listed on their literature as a Hallux Valgus shoe and at the time of my purchase was 45 euros . They were literally lifesavers and I am so grateful to them. These special shoes work by keeping the weight of the foot in the heel. It allows you to walk in a safe way, without disturbing the healing process or the new alignment of the big toe that the Surgeon went to great lengths to create. Goodbye zimmer frame! I got dressed, packed up my things and then I was discharged. A Nurse took me via wheelchair to the patient collection point of the hospital. A friend picked me up in order to bring me home. On the way home, we stopped vis the Pharmacy to pick up the anti-coagulant injections. They kindly took my dog out for another walk (they had been walking my dog for me whilst I was in hospital). They also offered to come for a few more days to walk the dog as they could see that I was quite incapacitated. I was in a lot of pain but absolutely delighted to be home. We always heal faster at home. I had already stocked up on easy to eat food items before the operation. I set up a big drinking bottle and water dispenser on the kitchen table. I still had the animals to feed and myself to take care of and that was a difficult enough chore post surgery. I realised that I would not be able to get in and out of the bath, as it has a curved edge and proves to be quite an ordeal when both feet work. I placed a low plastic foot step in the bath and a chair next to the bath. I got some plastic bags to protect my foot from splashes. I had changed my sheets the morning of the operation so that I would have the best hygienic environment for my freshly operated foot to rest in at night. I also had a freshly laundered bath towel to hand. I would say the first few days were the worst - sleep was very limited. I used a small pillow under my foot at night. For about a week I could only sleep on my side with the outer edge of the operated on foot making contact with the mattress. I had to take a neck pillow with a button (for transportation) and lightly fasten it around my ankle to help absorb some of the weight of my foot whilst in bed. After a week or so, I could lay on my other side if my foot was in a certain position - without any pressure on the site of the operation incision or above the Osteotomy site. I elevated my foot on and off throughout the day for a good 10 days. I made sure that my foot was higher than my heart and that there was not an obstruction behind the knee. I started researching about foot elevation. I read something that really inspired me - it was about not elevating the foot too high as circulation would be impaired and to find a balance between time to elevate the foot and moving. Studies had shown that moving was beneficial to reducing oedema. I bared this in mind but also found that too much time on my feet made my foot swell even more. I was sleeping a lot during the day in-between doing the tasks I needed to do. I just did what I felt I needed to do to help me recover from the operation and from being on my feet post surgery. Two days post operation I had to get the dressing changed at the Outpatients Department. I finally got to see what my foot looked like and to find out more about what the procedure actually entailed. The Surgeon explained that he had removed a piece of bone from the metatarsal bone shaft and cut a ligament in-between the first and second toe. There were two incision sites - one approximately 3 cm one on the medial aspect of the foot (in line with the base of the toe) and one in-between the big and second toe where the Surgeon entered to cut the ligament away as it was too tight and it would have pulled the toe offline. He also explained once again that all of my toes were out of line at the MTP joints and that procedures would most likely be needed to address this. The side of my foot looked notably flat and I was pleased with the visual outcome (not that that had been the main factor in me electing for this operation. The Surgeon explained that there was still plenty of swelling and that the final result would look even better. The Surgeons also encouraged me to try and walk more naturally with the Surgical shoe as it was designed to assist me with the walking action. This was something that took me a good week or so to get used to. My gait was shorter, there was inflammation and I was in pain; it was very difficult to relax and attempt to adopt a more natural walking gait. This did come in time though... I was given a sick-leave note for 6 weeks. It was a shock to see the rod sticking out of my toe. I recall the Surgeon saying they had used Kirschner wires and when I Googled this, it came up with internal smaller pin-like wires that were subcutaneous (under the skin). This was a substantial rod...sticking out of my toe by a good centimetre. A Kirschner wire is a sterilized, pointed stainless steel pin used to secure bones together until they heal. Martin Kirschner introduced these in 1909 and they are commonly used still in human and veterinary orthopaedic procedures. You might hear them being referred to as K-wires. I immediately asked about the rod and how it is removed. The Surgeon said it is done in the Outpatients Department and they just remove it without any anaesthetic or sedation. He said that there are no nerve endings within the bone and it is a painless quick procedure. They hoped that the wire could be removed in 6 weeks. The original surgeon told me 4 weeks, but I think the procedure I had done was more substantial than they originally anticipated. I also read that as the fracture heals, the wire becomes easier to remove as it gets looser. Another article explained that a sign that the wire is ready to be removed is that the fracture ceases to be tender to touch when palpated. Post removal there is often some bleeding and a dressing needs to be applied and kept dry. There was swelling present - especially at the lateral aspect of the foot and this was no surprise as I tend to rest on this edge of the foot. The toe was swollen, but not as much as I thought it would be. My original Surgeon who could not do the operation, as mentioned earlier, said that the new procedure that they perform tends to have less swelling. The wounds were wiped with gauze saturated in a clear solution. Then they were sprayed with a silver solution. Gauze was applied around the toe, in-betwen the toe, and at the larger incision site. Flat gauze was wrapped around my mid-foot. Pads of gauze placed over the area where the rod was protruding. A comfy padding was wrapped around my foot and an elastic bandage used to secure everything in place. It felt comfortable and pleasantly secure. As I started to move a bit more, the dressing started to move. My research told me that it was important not to restrict the area of the mid to fore-foot as this could impair the healing alignment. I used a bit of zinc oxide tape to secure the bandage in strategic places to avoid causing a problem with the healing process. This was too uncomfortable and I had to remove most of the zinc oxide tape - it was not a good idea. Micropore paper tape is a better option as it is lighter and less restrictive - especially important during this early healing process when swelling fluctuates throughout the day. You may need to let out the velcro on your Surgical shoe as the swelling increases to be more comfortable - make sure you get the support you need though. I also started to get some odd pains as the week progressed. It felt as if there was a great pressure between the toes and I wondered whether the dressing was digging into me. It was very intense. I know realise it was the stitches feeling uncomfortable as the wound was healing. There was general pain too - on top of the foot, at the site of the stitches on the inside of the foot, through the big toe, at the end of the big toe, under the foot and above the foot. I needed to take two paracetamol every 6 hours and literally counted the time down until I could next take pain relief. I would wake in the night in terrible discomfort. I could only have a few hours sleep and then I would need to get up and take pain relief. Sometimes I would need to take a good two hour break from sleep, wait for the pain to dissipate and then get back to sleep. The paracetamol did not stop the pain entirely, it did dull it down enough to be more bearable. I read something online about taking it slow after bunion surgery. It takes a lot of effort and energy to move around when you are in pain. Imagine what you have been through - the stress on the prelude to the operation, the preparations for your food, work, animals, children, family, the organisation of the home - linen changes, cleaning, gardening, the preparatory hospital appointments and so on. Then you have the sleep disturbances, food deprivation from the night before the operation, the dehydration, the medicines - spinal nerve blocks, sedation, pain relief, anti-coagulants, antibiotics, the stress of the pain, the stress of the operation on your body and mind - the incisions, the osteotomy (bone removal), the hole drilling, the rod insertion, the ligament release, the stitches, the inflammation and the pain. You have to look after yourself, the animals, the home, take care of welfare related paperwork and so on. You will be tired, not just because of what you went through, but also because of the healing process and life commitments post surgery. I had help with walking my dog for about 4 days before I realised that I needed to start walking the dog a little myself - how many favours can you ask from someone? This was hard for me and I was scared that I was creating damage - the Specialist said as I had the surgical shoe on, I did not have a limit on my walking. I could tell too much walking made the pain and swelling increase. Be careful walking when the ground is wet and uneven - the surgical shoe stops your proprioception from working as usual and it is easier to roll over your ankle and to slip. Also be careful being around, people and animals - you can predict your own movement to a certain extent, but not other living beings. Your foot is in a vulnerable state and you owe it to yourself and your medical care team to do your best to provide yourself with the most conducive healing environment. I also want to urge you to be utterly selfish and do what you need to recover. People will think that as you are home all the time, you have plenty of time and energy for visits. Well, no you do not. Everything you do will take double the time as you move slowly and carefully, and as you have to adapt everything you do - like washing your body and your hair, getting dressed, generally caring for yourself and so on. You will have medication to take and possibly side-effects from it. Your sleep will be impaired due to discomfort and pain. You will have to elevate your foot throughout the day. You will have lots of follow-up appointments at the hospital and lots of waiting around. You will need to sleep so much more than usual in the first few weeks to recover. You will be upset that your life has been completely turned upside down. Use this time to heal. Think of you. You are the most important person! A week later I was back in hospital having the stitches out and the dressing changed. I was surprised that the stitches were coming out so soon! They were removed easily and without pain. There was some bleeding due to the daily Enoxaparin Sodium Injections, which thin the blood in order to stop post foot surgery related blood clots. Apparently thromboembolic disease can be a life threatening factor post orthopaedic surgery because one is non-weightbearing and immobile post surgery. Luckily, with new surgery procedures and surgical shoes allowing bunionectomy patients to gain some mobility albeit in a limited and adapted manner, perhaps some of the high risk factors are offset a little. It was lovely to have a fresh dressing and bandage on again! The Orthopaedic Doctor (not my Surgeon) showed me the post surgery X-Ray and I was shocked to my core to see the big gap in the shaft of the metatarsal bone. I made a comment about the big gap and he said that they over-correct to ensure that the outcome is successful. I realised how fragile and vulnerable my foot was and how long the healing journey would most likely be and this was psychologically quite hard for me. I started to have nightmares about forgetting to wear my surgical shoe and losing it. Even during the day, I was worried incase I forgot post resting and put my foot down suddenly without the special protective shoe. 3 weeks after surgery, I had an X-Ray and bandage change. I had to arrive a little early to have the X-Ray before the consultation with my Surgeon. I was somewhat freaked out when the Radiographer asked me how I had been managing with my foot as it was. I realised that the gap between the two parts of the metatarsal had not closed and I became very anxious. My mind was racing back to two accidents I had had when I put my foot down abruptly when I slipped on the wet pavement walking the dog and also when I had accidentally put my foot down with some impact that had left me with much more swelling, pain and even numbness. The Surgeon said it was fine though. I was desperate to have the dressing changed as it was a good 10 days since the previous time. There was some bleeding on the gauze from when the stitches had been removed. Another weird sensation I started to have around this 3 week period was this restless sensation after being in bed for most of the night. As I was sleeping, I would start to move my toes and I would wake up due to the discomfort. One of the times however, I was in a deeper sleep and I must have attempted to move the toe a lot more and the lingering pain had me yelling out aloud for quite a few seconds. This funny sensation passed after a few days and just as well as moving my toes at this point in my recovery was a total contraindication and I was lucky that I did not cause damage. I was double pleased for the second X-Ray today! At 4 weeks post surgery I was back for another bandage change. I had not slept very well at all the night before. I had another accident with my foot and this time it was the worst to date. The evening before, I had been doing an online course and I was totally engrossed in the activity. The surgical shoe can get uncomfortable at times - even when you are just sitting the weight of the shoe can cause a little more pain. I could also feel that sitting still for a period of time had caused more swelling. So, I took off the surgical shoe and rested my foot on the table. I remember thinking that I must make sure that I do not forget and put my foot down... Moments later, I accidentally knocked my tea over and my laptop was in danger. I automatically sprung up out of my chair and totally absent-mindedly put weight on my foot without the protection of the surgical shoe. As soon as I realised, I got off the foot. The pain was sharp and intense. Instantly my foot and toe became severely swollen, my foot was numb and pulsing. The pain was agonising. I did not know whether to go to Accident and Emergency or even how I could get there. Luckily the next hospital appointment was scheduled for the morning after. I was embarrassed to tell the Surgeon what had happened. I knew I would have to... When I told him, he asked how it happened and said he would check it out for me. He cut back the bandage and dressing. The swelling was profuse throughout the foot and the big toe in particular - the Surgeon said that they were not worried about that. He said that he could see the toe was still in good alignment and that it was okay. He also asked how high my foot was when I put it down and he reassured me that all would be fine because of the metal rod they had inserted to maintain the correct post-surgery alignment. The Surgeon palpated the outer edge of my foot to see if there was pain and luckily there was not any. He did send me for another X-Ray though and told me to come back in to see them again immediately after. This Radiographer also made a remark about my foot and how painful it must be - she was shocked. I asked her if there was an improvement from the week before, and the original post surgery X-Ray, and she said that was something I had to discuss with my Doctor. When I was called back in to the Surgeon's consultation room, the two Doctors were double checking whether this X-Ray was from today. This made me even more nervous - was the healing delayed or did I cause any damage? Anyhow, they said it was all fine. There was still no union between the two halves of the bone, but it was evident that the gap was closing. I felt huge relief. I was extremely impressed with the care from my Surgical team. I also learnt a huge lesson - that unless I am lying down in bed, do not take off my surgical shoe! The really nice thing about today's visit was that I had a lighter more breathable bandage applied. This allowed more of my foot to breathe and stayed in place better. The next appointment was scheduled for two weeks time. They said I would most likely have the rod removed and that I would probably need to wear a toe splint. Also that I would not be able to return to my work yet as it is very physical. Now that the dressing was so much lighter and that 4 weeks had passed post-surgery, I started to do some lymphatic drainage techniques to assist with drainage from the swollen parts of my foot. This is linked to my work as a Professional Sports Massage Therapist - I would not advise that you do this at home, and definitely never without the permission of your Surgeon and the help of a qualified and experienced Physiotherapist. I also elevated my foot a lot more as per the first week post surgery - I was keen to recover from the accident I had. I also lightly massaged the scar. This is something that I have had much personal and professional experience with. When there is a scar, the dermal nerves can be damaged and can they can also elicit a heightened pain response. The scar tissue can also be prohibitive to natural movement - it tends to be restrictive due to the haphazard way it forms. It is important to restore function to the tissue and it is something that you do not hear much about. I used light longitudinal and circular frictions across the length of the scar. The pain was sharp, intense and almost unbearable - I used an even lighter touch until I found the sensation pleasurable. I actually felt that this might have been too early on in the healing process and aborted mission. Without the protection of the more padded dressing and bandage, the scar felt even more sore and raw. As the days passed, even just the contact of the surgical shoe became more tolerable - this must have been a form a desensitising in itself. I am coming up to 5 weeks post surgery and it is at this point that I really start to feel that healing is making better progress. The mid-foot / osteotomy area is less sensitive to touch, there is less sharp pain, I sometimes forget to take my scheduled pain relief and I am not waking up during the night in agony. I know that there is still a long way ahead of me to recover but I feel more optimistic. At week 6 I will be having another appointment with the Surgeon. I will update as I have more information, but the intention is that the rod will be removed. I have been thinking about the future and what I might do differently in the short and longterm. I am going to give away or sell my high-heeled shoes - I only wear them for special occasions if at all, but I still want to get rid of them just incase they re-aggravate my healing foot or cause a problem in the future. Some of the lower to medium heel height shoes with good support (ankle straps) I will keep. When I wear these shoes, I will have flats to wear until I get to the venue. I will make it my mission to find beautiful going out shoes that are flatter - even if I have to make embellishments for them myself. I will find shoes that always suit my foot shape. I will never wear uncomfortable shoes - even if I do not realise that the shoe is uncomfortable until I have worn it and a return is not possible - in this case I will re-home the shoe. I will keep my tibialis anterior relaxed with stretches - when it is safe in my recovery to do so and with thumb pressures across the length of the muscle (I have already been doing these as the surgical shoe keeps you in dorsi-flexion which shortens the tibialis anterior muscle). I will massage my own feet daily with body lotion after my shower and perform foot exercises for strength, dexterity and to help engage the arches of the foot. I will stretch out the two calf muscles and keep the achilles tendon in good condition. I will ask for advice from my Orthopaedic Surgeon on what I should and should not do to ensure the health of my toes and feet. AuthorHello, I'm Eva Evangelou, the UK trained Sports Massage Therapist behind Limassol Sports Massage. I have been practising bodywork for 19 years. My Clinic is in Limassol, Cyprus - a beautiful island in the Mediterranean. My Client's vary from professional athletes and recreational athletes to the general population - who tend to have muscle tightness related to some aspect of their lifestyle. I believe that our bodies tell a story and we can voluntarily choose to listen to the clues, giving due attention to what our body needs, or be forced to take action later down the line. Our fast paced lives often remove our focus from self-care. I hope my blogs provide you with some inspiration to bring you back to the wellness you deserve.
0 Comments
Top tips to counter neck and shoulder pain at home.Neck and shoulder pain is a subject close to my heart, as it is something that I had to deal with from a young age and most of my clients in my treatment clinic present with some type of neck discomfort. I have come to realise over the years that this issue is far more common than we think and that there is quite a lot that we can do to alleviate the symptoms and manage the condition. It is important to identify the triggers and understand that there will be ups and downs - but with the right approach, the ups can outweigh the downs. Before we proceed, it is important that one seeks medical advice before embarking upon any type of self-help measure. So, do go and see a physiotherapist or an osteopath for an assessment of your condition, or visit your doctor and see whether you need to be referred to an orthopaedic specialist. This will help ensure that you keep safe and ensure that you do not unwittingly aggravate a pre-existing condition. The neck is a delicate area of the body and due care and attention is required. Neck pain can result from a number of different factors. Some of these factors could include a physical activity that is aggravating the neck, long-term stress, sleeping position, work posture, general posture, repeated asymmetrical movements of the head and certain sports. If you have experienced physical trauma via an accident, even after being cleared by a medical professional as being fit once again, some muscles can remain tight through a protective spasm. Let us look at some of these in a little more detail. Activities that could be causing a problem could well include seemingly innocent things such as:
You may be thinking that we were made to move and so why could these innocent activities be causing an issue? Our muscle groups tend to work in pairs - with one muscle contracting/shortening and the opposite lengthening. This is a great arrangement, and is known as phasic or action muscles. It means that these muscles have the ability to be used for a long period of time, as the two opposing pairs take it in turns to work. However, when we keep performing the same movement or holding the same position, the muscles become more rapidly fatigued and they are given less than the ideal opportunity to recover. The body also needs time to adapt and become accustomed to activity and the loading placed on it. When the average layperson embarks upon gardening, DIY (Do It Yourself) or painting property, their body does not tend to have the opportunity to adapt to this type of boom and bust activity. The position the arms, neck and shoulders are held in is highly relevant too. Imagine painting the ceiling of one of the rooms in your house and your arms being held up overhead for a lengthy period of time; this will place a huge amount of pressure on your neck and could well result in the neck muscles becoming overly fatigued and tight, and a headache ensuing. Whenever we are carrying something heavy, there is often a huge loading on the shoulders and the chest muscles. Imagine carrying a heavy item, our arms are out in front of the body, the chest muscles actively engaged, as well as the shoulder muscles. When we load the chest muscles in this way, we can be causing the shoulders to anteriorly rotate and come forward. This can tug at the delicate neck muscles and put loading on the cervical vertebrae (the neck vertebrae). Carrying unequal loads can also place added stress on the neck as the shoulder girdle rotates and one shoulder is held higher than the other. Even carrying a heavy handbag on one shoulder can become problematic for the neck and shoulders over a period of time. It is important to evaluate our activities and be able to identify what might be triggering our pain. This can be harder to do than it seems - there is often a reluctance to to attribute our lifestyle to our pain, I guess we do not want to believe that our activity choices or that the general demands of life placed on us could be causing us pain. Long-term stress can be another trigger for neck and shoulder pain. When we are stressed, our body tends to go into a fetal position; the shoulders come forward and the hip flexors contract. Shoulders rise and become rigid - this in turn places a huge stress on the neck. One thing we have to be very aware of is that the position we hold our body in for a long period of time, can become a version of our posture that we carry throughout the day. Shoulders rolling forward can lead to the wrong tensioning between muscle groups; with some muscles such as the rhomboids and the mid-trapezius becoming long and tight, and pectoral (chest muscles) becoming tight and short/contracted. Also, when stressed over a long period of time, the body can get stuck in a heightened state of adrenaline. This is an automatic physiological response to an event that is perceived as being a danger. The muscles gain tonicity as they are preparing to work to lead us to safety - there is increased blood flow, the pupils dilate, the heart beats faster and so on. As humans, this response can linger long after the danger has passed. In the animal kingdom, animals tend to recover faster once the perceived threat has passed. The stress hormones tend to remain in our systems for longer; our sleep can become compromised, our ability to rest is impaired and further anxiety ensues. It is important to adopt practises to help us relax mentally and physically. Meditation, easy gardening chores, spending time in nature, listening to music, focussing on song lyrics, participating in gentle sports and physical activity, can help us to stay in the moment and destress the body and mind. As a meditation practitioner, I was taught that stress can leave the mind during meditation, but linger in the body for longer. I see this when I am massaging my clients - their body always tells a story. It is also possible to get stuck in a pain cycle when pain is not dealt with in a timely manner. There is scientific evidence to back this theory up. A delay in dealing with pain can make us more likely to have pain for a longer period of time. There is also the possibility that the pain alters the way we move, or limits our movement; which can have a multitude of consequences - including causing problems with our movement patterns and our posture, as well potentially leading to depression, sexual issues and a general reduction in wellbeing. Healthy movement is so important for us. Many of my clients are desk workers; they often sit for over 8 hours a day. Even when we seem to be inactive in a sitting position, we still have muscles that are firing to help us keep in that position. The hip flexors are working alongside the extensors of the back, the pectorals, the trapezius and the sternocleidomastoids. In a poor desk sitting position, the weight of the head places pressure on the delicate neck vertebrae - in fact, the loading on the neck increases the lower the head is held. This can get even more challenging when two computer screens are used - especially when one screen is looked at more than the other. It is important to have the main screen positioned centrally ahead of you. Repeatedly turning your head to one side can create an imbalance in neck muscle tightness. I often get my clients to think about how their television viewing station is set up, as well as the dining area and the socialisation area - looking straight ahead when there is neck pain is key, especially in the recovery phase. We want the neck muscles to fire evenly between the left and right sides, and the front and back of the neck. Think about your posture throughout the day. Are there any activities that leave you with one-sided neck pain? Is your television screen straight ahead? How about your dining table seating arrangements - is the company you keep sitting next to you or opposite you? At work, do you have your colleagues always approaching you from the one same side because of your desk set-up? Do you balance your phone against your ear and shoulder? Start to be aware of your body throughout the day. Take note if anything that you are doing is having some kind of negative impact on your body. Sometimes the effect of a repetitive or one-sided movement can take a bit of time to show - if there is neck pain, look back over the last couple of days to see what could have been a triggering factor. How about looking at our sleep posture? Is your pillow right for you and your personal anatomy? Is the pillow thick enough for the width of your shoulders? Your neck and your vertebrae should be in a straight line as you are sleeping - get someone to check this for you. Some people enjoy using anatomic pillows as it helps support the neck alongside the head - these can take a bit of getting used to. Memory foam pillows of varying firmness can also be popular. People tend to need to go through a few before they find the one that suits them best. Tummy sleepers sometimes fare worse than back and side-laying sleepers, as their heads rest sideways to their prone body - which invariably puts a strain on the neck. It could be worth experimenting with having a pillow under the chest, or even a bolster under one of the arms. In an ideal world, one might try to change their sleeping position if tummy sleeping is leading to a lingering amount of soreness during the night or the following morning. On the topic of sleep, check that your mattress is not too firm or too soft, or too old and worn. A saggy mattress will encourage the hips to sink too far, altering the straight line we wish to achieve from the neck along the length of the spine. A worn out base could also have a negative effect by robbing the mattress of effective support. Are you warm enough when you are sleeping? During sleep our body temperature drops. In the colder weather it is important to make sure that you have a reasonable temperature in the bedroom and ample bedding that covers the vulnerable parts of the neck. Use a small soft blanket or a snuggly throw on the bed to bridge any small gaps between the bedding, your shoulders and your neck. Also watch out for draughts from open windows, fans blowing on the neck and air conditioning units blasting out cold air directly on to you, as these can upset the nerves and the muscles. Muscles that get cold whilst you are sleeping can go into a type of spasm. I see this regularly in my Sports Massage Clinic. Change the direction of airflow where possible and keep a light sheet over your shoulders. In Cyprus, I notice an increase in neck and shoulder related problems when the weather changes as fans and air conditioning units are used in the bedroom and at the workplace. What about our sporting activities? Is there anything that we do in the gym or during our workouts that can aggravate the neck and shoulders? There can be sports related triggers to our workouts. Some of these could be due to poor technique - consult with a properly qualified and experienced coach to have your technique checked and corrected, or even adapted where necessary. Some movement patterns might need to be retaught to use the correct muscles in the right order - especially if movement patterns have become altered. Sometimes, the volume of training might need to be reduced for a period of time until pain is under control. Once pain is under control, training can be gradually increased within the remit of pain and discomfort. When we are in the middle of a severe neck/shoulder pain cycle, it might not be a good idea to train muscles that affect the this area. There are a large number of muscles that support and help create movement in the shoulder and some of these can directly impact the neck. Overly tight and spasmed muscles can result in impaired and limited movement patterns. Tight muscles are more easily upset and can become upset further, or even damaged if a large load is placed on them whilst they are in a vulnerable state. It is good to move within the remit of pain, but not to overly challenge tight muscles during a pain crisis. Once again, get pain under control first. Some examples of physical activity that might impact the neck include overhead cardio-inspired punching drills. Sit-ups - there are many kinds and various ways to adapt them to make them more user-friendly. Back extensions from a bent over flexed position. There are more - you need to explore to find your own triggers. Whatever happens, you are the first person to gauge whether something is causing you pain and if the adaptation is suitable for you. That inner voice inside you, that you learn to block out, can be the warning that you need to take heed from. Be brave enough to speak out and ask for an alternative exercise or to just skip certain exercises for the meantime - until things are back to normal for you again. Can clothing have an impact? Yes, in the summer, there are many garments that can upset the neck around the C7 area (where the vertebrae sticks out at the base of the neck). Halter neck bikini tops, casual tops and sports bras with high up racer backs can put pressure on the delicate neck vertebrae. When should you get help? If there is any pain that lingers, gets worse or disrupts your daily life, it should be investigated. Types of pain/symptoms to look out for include intense migraine like headaches, neck pain, shoulder pain, blurred vision, nausea, stiffness in the neck and upper spine, neck muscle spasms and restricted movement of the head. If there is any numbness in the fingers or thumbs one should seek help as this may be indicative of a nerve related issue. Look for postural imbalances - are the shoulders at an even height, is the chin jutting forward, are the shoulders rounded and coming forward? It is always best to see a medical professional in the first instance anyhow - whether that is a Physiotherapist, an Osteopath or an Orthopaedic Specialist. Seeing a medical professional on the first instance also allow Sports Massage to be performed in a targeted and safe manner. Pain should be addressed as it can be an indicator of a medical issue or a sign that we need to make adjustments in our life - especially in our daily self-care and in the general balance of our lives. The concept of The Three T's is close to my heart. When muscles become unhappy, it is often because we have done Too Much, Too Soon and Too Fast. People do not tend to like this when I tell them - especially when it is related to their sporting activity. The body always has a story to tell and it does not lie. When we train or do any physical activity, if we do more than our body is accustomed to, our muscles can become super tight and loose some of their flexibility therefore putting added stress on to the tendons - resulting in inflammation of the tendons. Joints can in turn become affected and also inflamed. Movement patterns and chains can become compromised and more issues can entail. We need to gradually build up the stresses and loads placed on the body - adding incrementally increasing physical stress, but also allowing time for the body to adapt, recover and gain strength. The best example of this is in the case of a runner who might run too many times a week before their body has become adequately conditioned and at a pace that is too fast. The Three T's can be applied to any physical activity. What you can do? - Basically you have three options. 1. Avoid the activity that is aggravating your neck (not always appropriate or fun). 2. Adapt the activity in some way to have a less harsh impact on the body. 3. Do damage control to offset the impact of the activity on your body. Keep a journal to help you become aware of what your triggers might be - briefly note down what your activity was along with a morning and evening pain scale rating from 0-10 (0 = no pain and 10 = extreme pain). Seeing an overview of how are you doing may help you to find triggers that you may have otherwise not taken much notice of. Get a massage from a professional with specific training such as a Sports Massage Therapist or a Rehabilitation Therapist. They can help identify any muscular imbalances and give you a stretching programme to help address postural related issues. They can also advise as to whether any muscle groups need to be strengthened. Specialist massage is great for helping to address the balance between muscle groups and help the joints move a little more freely. You may also consider carefully using a massage tool - always avoid too high an intensity, working over any bones, and using it for too long or too frequently. A tennis ball in a long sock can also be used for trigger point work - stand against a wall and lean on the ball in the area of any tight muscles on the back of the shoulder blades, or in-between the shoulder blades. Stretching and mobilising the neck and shoulders can also be useful in reducing pain symptoms. Gently turn your head to the left and the right - try to increase your range of movement. Try taking your ear to your shoulder laterally - do you see a difference in movement capability between the left and right sides? Stand with your back against a wall and lengthen your neck by taking your chin back - enjoy the stretch along the base of the neck. Squeeze the shoulder blades together using about 20% effort - this will help open out the chest and re-educate the muscles in-between the scapula to give you better postural support. Stretch out the pectoral muscles of the chest with a door frame chest stretch - stand in the doorway and hold the door frame with both hands whilst you gently allow the body to fall forward. Hold stretches for the neck for 10 seconds and the chest for 20 seconds - 20 is the ideal time, but I find it can be a bit harsh on the delicate neck area. Experiment with laying back on an arched back stretcher or a yoga bolster - this is great to counteract poor posture, decompress the spine, relax the muscles and to open out the chest. If symptoms increase stop performing or modify these tips. AuthorEva Evangelou is a Sports Massage Therapist with over 18 years of bodywork experience. Her private practice is in sunny Limassol, Cyprus. This Blog is based on her findings in her Massage Clinic and through her own experiences with battling chronic pain and various sports injuries.Write something about yourself. No need to be fancy, just an overview. What are the signs that we may be over training?
This blog is coming to you soon This Blog is coming to you soon
We have been qualified to apply Kinesiology Tapes (also known as Elastic Therapeutic Tapes) and Fixed Tapes for a few years now, following additional training at St Mary's University, Twickenham. It rapidly became one of our favourite methods of treatment in our busy Limassol based Sports Massage Clinic because of the success we have had with it. Why does Kinesiology Taping prove to be so helpful? The reasons are not scientifically proven. It is thought to help with the fascia by lifting the skin and giving the muscle and fascia a little more comfort. It is thought to keep the area a little warmer, to give a little support (depending on the way it is applied) and to help one remember that they have an injury that they are rehabilitating. How has Kinesiology Tape helped our Clients? We have used these tapes in a number of treatment applications. They have helped Marathon Runners as part of their treatment for Jumper's Knee/Patellar Tendinitis, Achilles Tendinitis and Iliotibial Band Syndrome. These runners had injuries resulting from doing too much, too soon in training and their races were at risk. Following intensive Sports Massage Therapy, they were taped for periods of two weeks. The taping helped prolong the benefits of the treatment and allowed for assistance with their recovery. Runners were taped for their races too. Other Sports disciplines/applications have included:
A Cyprus Ultra mountain race never passes without us taping some of the runners. It is usually helpful to tape the quad muscles to help them relax a little and we have used advanced techniques to tape a mal-tracking patella, which we believe saved one of the runner's races one year. Our running experience and Sports Massage Therapy knowledge has aided our understanding of application methods and has even allowed us to blend elastic and fixed tape for more effective treatment protocols in certain cases. Personally, I think that there is an additional benefit. I believe that the focus/awareness of the injured area helps to send more blood there. Increased blood flow can help with recovery and can bring healing agents in a more directed manner to the site of injury. It has been proven that focusing on an area of the body sends more blood to it. How is Kinesiology Tape applied? There are often several ways of applying elastic therapeutic tapes. Main principles include stretching the muscle whilst it is being taped. Tape edges are rounded to help them stay in place. The edges of the tape are not stretched; in order to ensure that they adhere well. The main section of the tape is stretched a certain percentage, depending on the area and the desired outcome of tape application - it is not stretched 100%, but 50-70% is very common. The tightest part of the muscle is often the part that the tape is first attached to. Whilst some knowledge of the path of the muscle in question should be understood and followed, there is not really anything that you can do wrong with elastic therapeutic taping; it simply will not be so effective if it is not positioned correctly. Kinesio Tex Classic - for great quality and the ultimate staying power:
Rocktape - for quality and performance:
Mueller Kinesiology Tape - value and performance
Levotape - doing a jolly good job!
Which brand? There are the expensive, and believe me you do get what you pay for, and the moderately priced. Go for a mid-price to expensive brand. Look at brands such as Rocktape, Levotape, Kinesio Tex and Mueller. You will love all of these brands. Check them out via the links above and order your preferred tape with ease. Pre-cut tapes are more expensive and whilst being convenient, are limiting in terms of their predetermined length. If you would like to buy tape in Clinic, we often have some in stock. Taping can be used as part of your Sports Massage treatment if we deem it useful, or can be booked as a treatment separately with a fee payable to cover materials and our Clinic time. AuthorEva Evangelou IFA & ITEC Diplomas in Sports Massage Therapy, Anatomy & Physiology, Clinical Aromatherapy and Holistic Massage Therapy. Education Adv Diploma, PGCE & BA Hons. Shin Splints can make your training programme a misery, read on for some tips to help combat this condition. Debilitating and painful, shin splints tend to come on when we have increased the demands of our training without pre-conditioning our lower leg muscles. Runners often suffer if they increase their mileage on hard ground, or up hills too quickly. Walkers can suffer with sudden increases in distances. Gym users who suddenly perform lots of explosive movements and 'on your toes' type exercises can get this condition. In mild cases it can feel like tenderness across the front of the shin that temporarily eases off with movement. In extreme cases, it can lead to fractures of the surface of the tibia (the load bearing lower leg bone). In fact, we have seen swellings the size of an egg on shins where this has unfortunately been the case. When shin splints present in such an extreme manner, complete rest from activity is required. In milder cases, and remember that catching sports injuries as early as possible is key, there are a few things that you can do to help with a smoother recovery. As soon as you feel tenderness across the front of the shin, try to rest from the activity that triggered it. A smaller rest at this point could save you from a much longer rest due to the condition deteriorating. Think about changing your sport for a while, or at least altering some aspects of your sport. It is best to avoid high impact activity until symptoms subside. When you have a sports injury type niggle, you have three options; to stop whatever is causing you a problem, to modify the activity, or to try and deal with the symptoms (the latter works best if you catch the injury sooner rather than later). Taping the Tibialis anterior muscle can be a good option too. Zinc oxide tape can be used to draw the muscle away from the shin bone in a spiral fashion during rest phases. If exercise continues, the elastic therapeutic taping methods are better. Speak to us in Clinic about which method will suit you better. Stretching the Tibialis anterior muscle is very helpful. Sit on your heels in a kneeling position for 20 seconds. Try this for two weeks at least 5 times per day. There are more advanced versions of this stretch available too. Sports Massage Therapy is ideal for this condition. Releasing the muscles in the lower leg and using specialist techniques to stretch the Tibialis anterior muscle is very helpful. Try at least three sessions over two weeks and follow the home-care advice carefully for optimal results. Try some ice therapy in acute phases. Just 10 minutes at a time on a small localised area a few times a day. This is especially useful post activity. Pre sports, apply a warm compress to allow the muscle to soften and relax a little. When you are symptom free in walking for at least two weeks, you can go ahead and slowly reintroduce some exercise in moderation. Do not do too much, too soon or too fast as your symptoms will return very quickly. When you are back to very light training and symptoms are symptoms are not present at all, you can add some very basic strengthening exercises. Be aware that rehabilitation exercises are very different to training exercises and they may appear to be easy for you but that is okay. Speak to a Personal Trainer with a rehabilitation qualification for assistance. Try toe raises whilst sitting. Aim for 10 raises per day for two weeks and when this goes well, without symptoms, move on to two sets from week three onwards. Calf raises can also be helpful, do these without weights and be extra careful to build up slowly. Try 5 slow raises on two legs for two weeks. If symptom free move on to single leg raises from week three onward. As always prevention is better than cure. Be hyper vigilant for small aches and pains, watch out for any tender areas and allow enough recovery time so you have a better chance of keeping repetitive injury free. AuthorEva Evangelou, BA Hons, PGCE, Adv Diploma, ITEC & IFA Dips, is the UK Qualified Sports Massage Therapist behind Limassol Sports Massage. Being a Qualified Sports Massage Therapist has given her extensive training and experience in Injury Prevention, the Theory of Training and Injury Rehabilitation. She has been a Body Worker since 2004. Eva has run 3 full Marathons including Nicosia, Rome and the Limassol Marathon. She is usually injury free and believes that prevention via education is better than cure. She is the Author behind 'Say No! To Neck and Shoulder Pain' and she is a Qualified Teacher. Learn more about her at www.LimassolSportsMassage.com and contact her via [email protected] Tearing your meniscus cartilage in the knee can be a very painful and debilitating injury. We know this first hand, as we have a severe and a moderate tear in each knee. It does not always mean surgery is required, even when it is recommended to us by our Specialist. Read on and get down to your Sports Physiotherapist for some assistance. Meniscus Tear Rehabilitation In the first instance of a tear, you will need to get medical assistance for a correct diagnosis and advice for the best way forward. Treatment can involve surgery if the knee is locking or there is advanced age/activity related degeneration. Loose cartilage can be trimmed and in some advanced more costly operations, some replacement can be made (just think of some of our elite athletes especially in first division football) . The first port of call is to reduce inflammation. Ice 3 times a day for 10 minutes at a time across the front of the knee. Wrap a pack of frozen peas in a damp tea towel. Never ice around the entire knee. Never exceed 10 minutes of icing at a time. Repeat as much as you like, as long as the tissue has returned to its original colour and tone. If you have access to a swimming pool, water walking is great for reducing inflammation. Keep repeating until swelling subsides completely. Repeat as needed if swelling returns. 2. Tape the patella if it is suspected of mis-tracking. When the knee is injured, the quad muscles often lose their ability to anchor the patella adequately. Taping the knee cap to anchor it more medially is often a good idea. Use elastic therapeutic taping as it still allows unrestricted movement. Kinesiology taping can be used for up to 5 days at a time if no allergy is present. Remove the tape slowly and carefully to avoided irritating the skin. Aim for two weeks of taping with a couple of days off to let the skin recover when the tape is due for a change. Stop if the skin is irritated. 3. Quadriceps stretch (front of thighs) Grab hold of your ankle, take heel to bottom and keep your knees together. Repeat for other side. Perform again for the tighter quad. Do this stretch 5 X a day for two weeks and then review. We need to keep the quad muscles supple. If you find it hard to kneel, you need to keep practising this stretch. Hold stretches for 20 seconds. If one side feels tighter than the other, perform the stretch again on the tighter side. When you feel symmetry, perform the stretch once per side. Only perform when warmed up later on in the day. Modify if discomfort is present and stop if there is pain. Stretches should feel comfortable. If there is any shaking, release the stretch and attempt again with less effort. 4. Strengthen the medial quad muscle with wide legged squats. Perform two sets of 10 twice a day for two weeks. Get a PT instructor to check your form if you are unsure, but aim to keep knees over the feet. A small range of movement is acceptable until you are able to get a little lower (never lower than 90 degrees however). 5. Try a single leg squat for the affected leg with a support strap to take most of your weight. Only do this if you have a strong and supportive strap/anchor. 2-5 X single leg squats once per day for two weeks. 6. If you have access to a gym, try a single leg press with the affected leg. Keep your foot flat against the platform and keep the weight very light indeed. 5-10 presses per day for two weeks, or for at least three days per week until you gain strength. If there is pain, modify a technique or stop using the technique. 7. Practise flexing and extending the knee. Start off by sitting on a tallish stool, and straighten and then bend the knee in a slow and controlled manner. Perform 2-4 times a day for two weeks. This can be done whilst standing and holding on to a surface for support. 8. Develop your proprioception by standing on one leg for 10-20 seconds. When this is easy, try it with your eyes closed; but have something to steady you close-by, in case you lose balance. This exercise will strengthen your leg/ankle and re-develop any balance issues arising from the injury. 9. Other tips
The overall aim of the programme is to:
This combination of flexibility and strength is key to managing most injuries. After two weeks of rehab review your progress. Is there any lingering inflammation? If so, continue with the icing and water walking. Is your knee feeling more comfortable? Can you feel the quad muscle on the inner knee getting stronger? Add another set of quad squat repetitions as long as there is no increase in pain. Continue for another two weeks and then review progress again. It can take three months of rehab to get to a more functional knee position once again. Then it will be a juggling act to maintain your progress, by keeping the quad strong and flexible, and being super vigilant for any inflammation flare ups or aggravating activities. Be aware that when you do return to activity, build up slowly and carefully so that your body adapts without any issues. AuthorEva Evangelou, BA Hons, PGCE, Adv Diploma, ITEC & IFA Dips, is the UK Qualified Sports Massage Therapist behind Limassol Sports Massage. Being a Qualified Sports Massage Therapist has given her extensive training and experience in Injury Prevention, the Theory of Training and Injury Rehabilitation. She has been a Body Worker since 2004. Eva has run 3 full Marathons including Nicosia, Rome and the Limassol Marathon. She is usually injury free and believes that prevention via education is better than cure. She is the Author behind 'Say No! To Neck and Shoulder Pain' and she is a Qualified Teacher. Learn more about her by clicking here and contact her via email by clicking here. We just read a fantastic , and quite alarming, article written by a leading Medical Journal about our heart and how it is impacted by stress. Stress and the risk of a heart attack, or cardio vascular disease is a subject close to my heart. Massage Therapy and Aromatherapy are good stress reducers. I see many people who are dealing with high levels of stress. Many of my Clients have had issues with their cardiovascular system. So many of my Clients are subjected to long periods of stress. As a Massage Therapist, I am well aware of the fact that stress can release bad cholesterol in to the blood stream. The pains we feel in the chest during long stressful periods, can in fact be linked to the blood vessels constricting; probably due to our fight or flight mechanism, but none-the-less being in a constant state of high adrenaline is wearing on the body and leaves it very confused. When we are constantly stressed, we can not sleep well, we tend to drop exercise as we are too exhausted, or we exercise and feel even more exhausted, we stop eating so well, we can not relax effectively, all our worries seem worse, our body is in a constant state of red alert and we let go of the support systems that can help us ease the burden of our stress. Over the years I have had more than my fair share of stress. I have even witnessed heart related issues within my family. There seems to be pattern linked to cardiovascular disease; the common pattern of elevated blood pressure, a reduction in stamina and heart rhythm alterations. I have often wondered why? Could it be due to bad genetics? Poor diets? Perhaps a lack of exercise? I have often pondered this question and now I have the answer. We are all great thinkers, or should I say worriers. We tend to worry about situations that we often have little control over. There have also been prolonged periods of stress in our lives. This can be quite a subjective issue and I believe that there are gender differences in how we perceive and deal with stress. I was most intrigued to find this article about stress click here and new evidence to link it with an increased risk of an heart attack. There was a study by a Harvard Medical School team of nearly 300 participants. Their amygdala activity was monitored. In the patients with higher activity in the amygdala, they were shown to be more at risk of developing heart disease. The amygdala processes fear and anger emotions. Heart attack risk factors were thought to be increased by the usual culprits of smoking and elevated blood pressure. The study now added a new factor to that list, stress. Stress including emotional stress. Chronic stress can be induced through over work, living in poverty, work-related issues and so on. Emotional stress affects the cardiovascular system by affecting the heart and the blood vessels. The Lancet Medical Journal studied 293 people over 4 years. 22 of these people developed cardiovascular disease. All of these people showed higher activity in the amygdala. Those that reported higher levels of stress in their lives, had higher levels of activity in the amygdala and more inflammation in their blood and arteries. If stress can be reduced however, there is a lower chance of cardiovascular disease developing - that is now a fact. How can we reduce our levels of stress? We can have Massage Therapy, develop a regular exercise regime, take up meditation, spend time outdoors, find a good non-judgmental listening ear when we have issues and make lifestyle changes. Eat natural foods, drink less or avoid alcohol, make work less stressful, get your finances in order, associate with friends that are good for you, get enough sleep and keep healthy relationships. Aside from all of this tips, I guess we need to adopt a bit of a lighter attitude towards life too! Authorva Evangelou, BA Hons, PGCE, Adv Diploma, ITEC & IFA Dips, is the UK Qualified Sports Massage Therapist behind Limassol Sports Massage. Being a Qualified Sports Massage Therapist has given her extensive training and experience in Injury Prevention, the Theory of Training and Injury Rehabilitation. She has been a Body Worker since 2004. Eva has run 3 full Marathons including Nicosia, Rome and the Limassol Marathon. She is usually injury free and believes that prevention via education is better than cure. She is the Author behind 'Say No! To Neck and Shoulder Pain' and she is a Qualified Teacher. Learn more about her by clicking here and contact her via email by clicking here. Get in shape with the outdoor fitness coach and personal trainer Michael Rivers for a fun and effective training programme. To find out more and to book a try out personal training session in Limassol, visit www.michaelrivers.com Telephone +357 95508007 or email [email protected] Hello dear Limassol Sports Massage supporters,
The weather is characteristically windy for this time of year. One of our dear Clients gave us a chart with Coptic gale and wind storm predictions, and we due to receive three this month; which we are experiencing greatly indeed. This is not so helpful for those of us who love our outdoor sports as the air is full of dust and allergens. We are pleased that the Limassol Marathon has been moved to April this year as the wind proved prohibitive in the last few years; they even had their administration tents blow away! We continue to write for the Limassol Marathon as their partner 'Expert Writer'. You can see a selection of our sports related articles here. The Limassol Marathon is on 10th April 2016. It is a wonderful event. Do come and support the runners - all cheering and clapping makes their efforts even more rewarding. For those who would like to volunteer, send the organisers a message through their website contact page. There is a special event aimed at Women in Limassol this weekend (March 19th/20th) at the Elias Beach Hotel. There will be two days of talks, music and exhibition tables by Women for Women for just 79 euros. A one day ticket at 49 euros is also available. If you use the code 'LimassolSportsMassage' at their website here and you will get 10% off all ticket prices. Have a look at the website for the Conference Schedule. We went last year and supported the event as Limassol Sports Massage. We donated our signature blend 'Lavender Spritz bottles' for all attendees and made a donation on behalf of Limassol Sports Massage. These events do not come up very often in Cyprus and they are a special way of reaching out to other Women on the Island and learning about their hobbies, health stories, business industries and individual success stories. The Cyprus Ultra Marathon in Vasa Kellakiou has just announced its next big race date, which is May 20th-22nd 2017. We will be offering our services to help organise and direct the race as per usual with next year being our 6th Cyprus Ultra! We expect participants to reach the 200 threshold. Ticket sales have got off to a good start with ultra low prices for the early entries. We have many runners returning for the third time as the race has such a family feel. Plans for next year include a camp party open to all well-behaved revellers on Saturday night and activities, including field games and traditional food dishes, with a village fair theme. If anyone would like to register for the race, there are distances available to suit all levels of running, have a look here. We are also calling for Volunteers. You will be working very hard in the May heat (shady areas are available for those who need to keep out of the direct sunlight), but the work is greatly rewarding. We have Volunteers coming back for the sixth time and new Volunteers every year. If you can spare a block of 4 hours or more, or even if you want to camp out with us for the whole weekend, please get in touch on 99231970 - food and water will be provided. Having patience and a good sense of humour is a must! Our partners V1Fitness have just launched their new self-defence Limassol training packages and we have been trying out their latest moves. Check out their webpage here and see if it is something that you or your loved one would like to do. Much of self-defence is about awareness and having the right initial response if an attack occurs - you will love the no-nonsense approach of this self-defence system and the levels of fitness it helps you achieve. Check out their new training dummy on your next visit to us! Giving this guy a bash in the face with a palm strike is a great stress release indeed! Contact Mike on 95508007 for more information and visit his website V1FITNESS.COM There is plenty going on this Summer. Mike is offering Rollerblade Inline skating lessons at Molos for individuals and small groups. The Limassol Running Club has three runs per week with free accessibility to all. We are also planning a few walking hikes in the mountains too. Do get in touch for more information on 95508007. We have just ordered more Kinesiology tapes which will be available in Clinic again very soon. We have also ordered the supplies for our in-house MSM Aromatherapy muscle gel and our original Aromatherapy Muscle Gel too - we shall let you know when these fresh batches are ready for sale again at 20€ and 15€ respectively. We have had great feedback about these gels -with Clients reporting pain relief and a reduction of inflammation. We are getting quite a telling off for running out of stock - one Client even threatened to try and make their own if ours were not back in stock again soon! Our 'Say No! To Neck and Shoulder Pain' book is now available in Cyprus Libraries and will be on amazon.co.uk by the end of the month hopefully too. Sales are off to a good start - you can pick up your copy in Clinic for 10€ or online click here with PayPal (P&P fees and PayPal charges apply for online sales) Wishing you all a good start to your Sporty Spring and see you all soon! Kind regards, Eva from Limassol Sports Massage |
AuthorSports Massage Therapist, Wellness Advocate, Sports Enthusiast, Teacher, Nutritarian, Blogger, Artist and much more... Archives
October 2022
Categories
All
|

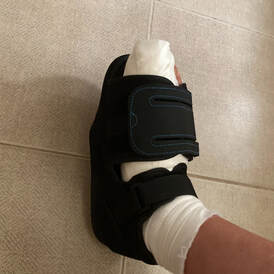
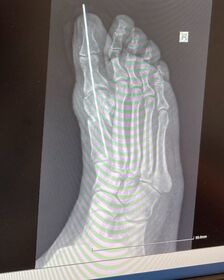













 RSS Feed
RSS Feed